 The primary service we provide at Austin Skyline Dental is taking care of our patients. Along with the actual clinical procedures we provide, there is an above and beyond effort to take care of those extra details. Such things as expediting lab times, providing occasional transportation for our non-driving patients, and even a little “day care” while mom receives treatment is our style.
The primary service we provide at Austin Skyline Dental is taking care of our patients. Along with the actual clinical procedures we provide, there is an above and beyond effort to take care of those extra details. Such things as expediting lab times, providing occasional transportation for our non-driving patients, and even a little “day care” while mom receives treatment is our style.
From the standpoint of dental services, we focus on patient education, decay prevention, restoring teeth, maintaining healthy periodontal tissue, providing excellent cosmetic results and helping maintain harmony between the occlusion (bite), the chewing muscles and the temporomandibular joint (TMJ). Our doctors have attended extended cosmetic continuums and excel in smile design. As members of the American Dental Association, we are pleased to provide the educational program PATIENT SMART, attached to this website. PATIENT SMART provides an explanation of dental procedures in general. Please feel welcome to browse this information source.
List of Dental Procedures:
It is often in our patient’s interest to repair their existing removable appliances rather than building new ones. We help coordinate our dental laboratory to restore existing appliances, usually within two working days.
This is the process of smoothing sharp or prominent edges on the bone that supports our teeth. An alveoplasty is most often needed when several teeth in a row need removing. This recontouring of the bone is blended together before suturing, resulting in a smooth edentulous ridge.
The long standing silver amalgam restoration is often a controversial topic due to the presence of mercury. We make certain to discuss this with each patient for whom we feel a silver amalgam will outperform the composite restoration we place far more often. The current science behind the mercury topic is that the mercury does not leak from the restoration. The American Dental Association continues to support the safety of amalgam through decades of longitudinal study. In our practice, no more than one out of every hundred restorations are recommended to be resolved with a silver amalgam. In these cases, allowing the amalgam often helps avoid the need of a laboratory crown. The amalgams we place are so far in the posterior of the arch (usually upper) that they are seldom seen. A small percentage of our patients actually prefer the security of a metal restoration. We believe the rule of the 99 is the 1.
A bridge is a fixed prosthesis, replacing one or more teeth. They are typically connected to two or more adjacent teeth for support. Unfortunately, too many times the adjacent teeth are healthy and have to undergo crown reduction just because they are next to the lost tooth. We seldom build bridges these days due to our high success in replacing lost teeth with implants.
This is where our passion lies! We build our own splints here and consider them a combination of art and science. Our protective splints shelter teeth from the accelerated wear and fracture susceptibility introduced by grinding (bruxing) as well as clenching. Splints are worn primarily nocturnally. We closely fit our splints to its supporting arch then precisely adjust the biting surface to the contours of the opposing arch. Splint delivery, followed by adjustments, usually takes about three appointments. (See TMJ Splint)
The case has been made for the durability of the gold crown for second molars. For those intolerant of the esthetics of a gold crown, enter the Bruxzir crown. Though not as malleable as gold, a Bruxzir crown is fracture resistant like gold. Unlike gold, the Bruxzir crown is tooth colored. It is not as natural looking as an esthetic crown but well passes as a tooth colored posterior crown. Bruxzir crowns are mode from zirconia, milled not cast. CAD/CAM technology is utilized and Bruxzir crowns are basically unchipable. (See Gold Crowns)
The term buildup refers to that high percentage tooth replacement filling that needs to be followed and reinforced by a laboratory crown. The buildup satisfies decay resolution but does not provide a long term solution for strength or resistance to recurrent decay. Ideally the lab crown process is started the day the buildup is placed, however, there are times when our patients need to delay or may be better served by delaying the laboratory crown. We use the term “phasing” to describe this process of first achieving health, following later with the longevity expected from a laboratory crown. To present perspective the expense of one crown would provide buildup fillings for four or five teeth. (See Phasing)
In addition our hygeniests’ mechanical cleansing of bacterial plaque and calculus from problematic deeper pockets, they place an antibiotic powder called Arestin directly into the pocket. Placing this minocycline (tetracycline) right where it is needed allows a concentration much stronger than could be achieved by oral/systemic antibiotics. Microspheres, smaller than we can see, slowly release the antibiotic for twenty-one days. Arestin can be placed either at the time of scaling and root planing or at follow up periodontal maintenance appointments. We closely screen our patients for the few that are sensitive or allergic to tetracycline.
Around the early 1980s, tooth colored composites became available to restore posterior teeth. Anterior teeth have had this tooth colored restorative material option much longer. The placement of posterior composites is surely our most frequent restorative procedure. We provide this service for health reasons, resolving both initial and recurrent decay. It is gratifying, however, to see a beautiful and natural looking result.
This is a surgical procedure to uncover tooth structure involving reduction of both gingival and supportive bone. Crown lengthening is indicated to eliminate “gummy smiles”, access decay near bone level or help in reaching further down a fractured tooth’s axis to better provide a laboratory crown. We diagnose and refer crown lengthenings to a periodontist. A high percentage of the time, however, we eliminate the need to refer this surgery through our definitive gingivectomy. (See Gingivectomy)
A shade guide is a series of “color tabs” representative of common tooth colors. This is the routine way a dentist communicates shade to the laboratory. Even with the best porcelain shade guide, there are only 22 shades. Compare this limited shade selection to the myriad of shades among our extensive base of patients and the hundreds of thousands of folks in Austin. The limited shade guide falls apart as adequate for important anterior crowns. On anterior teeth, we recommend custom staining with our master lab technician. We believe a cosmetic crown is a “durable good.” You will be seeing such a crown, in all likelihood, for decades. We believe custom staining is worth the extra time and minimal fee. Our achievable goal is for your crown to look natural. (See Master Lab Technician Blog)
Every once in a while, an older laboratory crown will dislodge from its tooth, usually due to recurrent decay…possibly assisted by sticky candy! If the crown can be reseated with adequate marginal integrity, we will work to help save the crown. We remove all recurrent decay then bond on the cleaned out crown. When appropriate, this pragmatic solution is most appreciated by our patients, avoiding the time and expense of a new crown.
Though conventional, old fashioned dentures don’t come along that often, we are comfortable in providing them for our patients. We often help our denture patients to dramatically better results with implants, underneath and supporting the dentures. Always looking to best serve our patients, we help some by referring those more complicated cases to a peer that is fully dedicated to this area of dentistry. (See Overdentures)
The chewing surface of the posterior teeth are naturally fissured or grooved. 80% of all decay starts in these grooves due to the retention of food particles and plaque.
The conventional methods of early detection of these areas of decay are disappointingly successful. These long standing methods of detection are visual, probing with an explorer and through x-ray. In our practice the visual aspect is enhanced with magnification and illumination but still falls short of the benefit of laser fluorescence.
Research documents the success of early diagnosis of these decays jumps from an average of 57% to 90% with the use of laser fluorescence. The instrument that provides this technology is the Diagnodent. This tool sends an innocuous laser beam into these grooved areas measuring reflected laser light energy. Clean, healthy tooth structure exhibits little or no fluorescence while carious or decayed tooth structure exhibits fluorescence proportionate to the degree of the caries. A digital display and audio signal quantify the degree of decay. This helps us make an earlier diagnosis.
Several years ago, when this technology was introduced to our practice, it was a leap of faith to believe enough to make a diagnosis based on the Diagnodant. On a tooth that showed no visual, tactile or radiographic proof of need, the responsibility felt in recommending a procedure was significant.
We are pleased to report that there has not been a false positive or unnecessary entry into healthy tooth structure over a sample in the hundreds by now. Conversely, there has been only the gratification of detecting and treating occlusal or chewing surface decay when it should be treated, in its early stages, with proportionately smaller restorations.
For approximately one fourth of our patients, archival models or casts are worthwhile. In cases of wear from grinding, cosmetic cases or those involving tooth replacement, nothing is better than accurate three-dimensional models.
As an important tool in our cosmetic philosophy, the diagnostic wax-up is a three-dimensional projection, utilizing carved wax to develop the ideal contours of the anterior teeth to be treated. This waxup starts with accurate diagnostic casts and begins the conversion toward that patient’s cosmetic ideal. The planning from the diagnostic waxup is a problem solving dress rehearsal of the developing cosmetic goal. The diagnostic waxup is the beginning of a pleasant metamorphosis!
We have never failed to respond to any dental emergency. This goes for both patients of record and new patients. Following resolution of our new patient’s emergency, they are offered our comprehensive exam. This thorough exam is the best we have to offer and every patient deserves it.
This is the proper term for root canal therapy. Our doctors routinely provide needed root canals, utilizing vitality testers, apex locators and rotary endodontic technology. Most often endodontics is a two appointment process. Dr. Kimball excels in this procedure and treats most of our patients’ endodontic needs. We, as well, readily refer more complex cases to endodontic specialists when it better serves our patients.
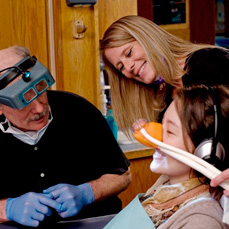
Enteral sedation is for those patients seeking more disassociation from their dental procedures than provided by nitrous oxide. Enteral sedation is achieved through carefully dosing our patients with Halcion, a sleeping pill related to valium. The Halcion is taken in combination with nitrous oxide and headphones. We administer the Halcion, dim the lights and about an hour later 90% of the time we have a sleeping but arousable patient. The use of a pulse oximeter and blood pressure monitor throughout, allows direct monitoring of blood oxygen levels for our patients. Those few that do not actually fall asleep have confirmed the effect is still adequate. Halcion sedation patients require a designated driver with whom we coordinate transportation following the appointment. But universally, amnesia is later described by our sedation patients. (See Nitrous Oxide Sedation)
Most porcelain crowns done ten years ago and back were fused to a metal substructure. To block out the dark metal, because porcelain is translucent, a middle layer called the opaquer was interposed. This opaquer succeeds at blocking out the darker, underlying metal but results in a crown that is flat or unnatural in appearance. We have all seen those laboratory crowns on front teeth that are unfortunately chalky, opaque in appearance, and obviously a “fake tooth.” We provide instead, esthetic restoration crowns without metal. They are beautifully translucent and “alive”, like a natural tooth. (See Custom Staining and our blog on the Esthetic Zone)
Extracoronal splints are present short term, usually for two or three months following accidental trauma, until the teeth restabilize. Loose teeth are stabilized by being bonded to stronger adjacent teeth. Since extracoronal splints are most often for anterior teeth, they are a cosmetic negative…but well worth it. Unlike the intracoronal splint, an extracoronal splint is based on an orthodontic wire bonded on the outside surface of the teeth.
We subscribe to the belief that safe levels of fluoride limit or prevent tooth decay. For over five decades, the American Dental Association has endorsed the fluoridation of community water supplies… Austin complies. Most toothpastes as well contain fluoride to reduce the incidence of decay. Our doctors administer prescription strength, therapeutic fluoride rinses when appropriate through our hygienists. We also prescribe fluoride for home use when indicated. We address decay prevention with stannous fluoride and hypersensitivity with sodium fluoride. (See Hypersensitivity)
Metal frameworks and metal clasps around supporting teeth have typified removable partial dentures for decades. The free resin system (FRS) partial dentures have zero metal, are flexible and much lighter by weight. Our doctors are very excited about the wearability of FRS partials. Everyone has seen those rather unsightly, dark metal clasps on conventional partials…not an issue with the FRS partial. Some of the more extensive partial dentures still require metal but we recommend the FRS option whenever we can.
We provide a gingivectomy for our patients when the area on the tooth needing treatment is under the gum line. Electrosurgery is employed to cleanly remove the interfering gum, accessing decay or allowing preparation of the otherwise subgingival margin for a laboratory crown. Gingivectomies do not include reduction of the alveolar bone but can go right to bone level. Time and again, our gingivectomies have proven adequate to get the job done, saving our patients crown lengthening surgery by a periodontal specialist. Seldom do our electrosurgery patients need prescription analgesics and the tissue regenerates in a healthy fashion within five to seven days. (See Crown Lengthening)
A cast gold crown is still an excellent restoration thanks to its resistance to fracture. The leading indication for gold is in crowning second molars, the last molar in position from the midline once your wisdom teeth are removed. We all chew our hardest on these teeth and conventional porcelain often fractures under such force. Many of our patients additionally brux or grind their teeth and the second molars take a beating. There is still no material better for this indication than gold. Our gold crowns are really gold in appearance, containing high gold content. (See Bruxzir Crowns)
Most everyone is familiar with advertised toothpastes for sensitive teeth. These over the counter products are successful in most part but inadequate in cases with overly sensitive teeth. There is no pathology involved in this condition appropriate to approach with restorative procedures such as fillings, root canals, crowns or veneers. We confirm any damaging bite forces are controlled and next address the symptoms of hypersensitivity. This is done with the prescription strength desensitizers potassium nitrate and sodium fluoride, as well as Gluma and custom desensitizing trays. Our help in controlling hypersensitivity is especially important for the approximately 20% of our patients experiencing sensitivity while whitening their teeth.
After co-planning for implants with an oral surgeon or periodontist, it is our job to restore the implant once it is stable in the bone. There are three components need for an implant crown. The first component is the implant fixture placed by either of these specialists. For the implant fixture to osseointegrate, or attach to the bone, takes about three to four months. Only after the fixture is anchored can we take our impression to restore the implant. We and our laboratory technician then select the second component, the abutment, which we secure to the fixture. The final component is the laboratory crown which is connected by the abutment to the implant fixture. The fixture, which does not show, is made of titanium while we can now provide metal free abutments and metal free esthetic crowns. (See Esthetic Crowns)
When a tooth is mobile, or loose, we work on the cause and can also place an intracoronal splint to stabilize it to stronger, adjacent teeth. Intracoronal splints are best suited for posterior teeth. A shallow groove is first prepared into the chewing surface of both the mobile and support teeth. As the name implies, an intracoronal splint is within the anatomic crown space of these teeth. An orthodontic wire is bent to fit into the groove and anchored into position by a nice looking composite filling material. Voila, all teeth stable again. An intracoronal splint helps avoid extraction of the mobile tooth and is intended to serve for a long time.
Maryland bridges are unique in requiring imperceptible reduction of the support teeth. This minor tongue side preparation of adjacent teeth allows the presence of “wings” or attachments, leaving the visible side of the support teeth unchanged. These bridges are only for the anterior portion of our patients’ dentitions. Maryland bridges do have a role in our restorative philosophy.
The time tested and safe use of nitrous oxide for sedation is important to our apprehensive patients. We carefully monitor the balance of oxygen and nitrous oxide for each patient to help them through their appointments. The nitrous oxide sedation provides different responses for various patients but, in general, allows our patients to disassociate, or mentally leave the scene. Especially with headphones, they leave the moment to moment tasks of the procedure, going into their own detached world. Receiving only oxygen and the ambient natural atmosphere for the last ten minutes of our procedure reverses the sedative effect. These patients are then able to drive safely to their next appointment or errand. (See Enteral Sedation)
A denture becomes an overdenture when it is connected through attachments to underlying implants or endodontically treated roots of natural teeth. These attachments connect the appliance to the supportive bone, improving stability and function. We have seen a night and day improvement for our patients versus soft tissue only supported dentures. No more denture adhesive!
Once treatment is under way, or completed, it is important to provide follow-up and monitoring. Periodic exams occur with hygiene appointments and are done at least once, usually twice per year. As months turn into years, changes occur in both our patients’ health and our technology.
You can’t prevent periodontal diseases once it is present. For our patients beyond a healthy gingival and bone baseline, we offer deeper pocket maintenance as part of our nonsurgical therapy. Following the scaling and root planing procedure, it is important to maintain the positive momentum of pocket reduction. To maintain this improvement, our patients of this profile come in for periodontal maintenance every three of four months versus semiannually. The benefit of more frequent hygiene appointments is validated throughout our periodontal literature. Should the periodontal disease remain uncontrolled, we are still timely with a referral to a periodontist. We do our best to help our patients avoid periodontal surgery, but on occasion it is indicated. (See Scaling and Root Planing)
Phasing is our term for attending to the more active needs right away, approaching chronic need treatment over time. Careful examination and treatment planning allows phasing to correctly help in both sequencing and budgeting. Phasing also allows compliance with the limitations of annual insurance benefits. Like it or not, these incremental benefits are part of the overall treatment equation.
As mentioned above, crowns of this type are no longer acceptable for front teeth due to appearing unnaturally opaque. In the posterior portion of the dentition, however, porcelain fused to metal crowns still have a role to play. The metal substructure allows reaching further down the axis of teeth problemed with more advanced breakdown. The edge strength of the metal allows it to be carried down even below gumline, reaching places nonmetal or esthetic crowns cannot go. Their intrinsic opacity becomes acceptable in these cases versus the cosmetic alternative of a gold crown.
Porcelain veneers are the centerpiece of our cosmetic dentistry, providing a conservative alternative to full reduction laboratory crowns. With veneers, a high percentage of tooth structure is preserved, yet still providing ideal cosmetics. Discolored, chipped, crowded or malformed anterior teeth are all correctable with porcelain veneers. Crowded anterior teeth, much of the time, can be cosmetically realigned as if by orthodontics. We work with an excellent esthetic laboratory technician, in part, because he custom stains our cosmetic cases. (See Diagnostic Wax-U, Custom Staining and our blog on the Master Laboratory Technician)
A percentage of the time, root canal teeth needing to be crowned require a post. The post is anchored in the filled canal space, connecting bone supported tooth structure to the build-up material which supports the laboratory crown. A post limits the chance tooth structure above the gum line will separate from the root portion of the tooth. Posts are done only when needed to provide a more secure foundation to hold the crown.
The majority of our patients are in the healthy range of gingival (gum) and bone health. Our job is to help them stay there. These structures supporting the teeth are just as important to remaining healthy as are the teeth. Oral hygiene instruction is added to the continuing care our hygienists provide. We strive to educate our patients of the cause and effect of gingivitis and periodontitis. We want our patients to brush and floss from a basis of knowledge, not reluctant obligation.
A pulpotomy is a partial root canal, usually done to help out on emergency patient. The pulpotomy stops the toothache, allowing rescheduling for enough time to properly complete the root canal. Pulpotomies are also appropriate for primary or“baby” teeth. These childhood pulpotomies allow maintenance of the primary tooth, providing interim function and more importantly, preserving the space needed for the upcoming adult tooth.
Since each tooth is a 5-sided cube and we can only see three of these surfaces, well-processed x-rays allow early detection of decay for those other two surfaces. Radiographs have numerous other benefits like letting us know what’s going on in the supportive alveolar bone. We believe in a thorough series of x-rays and keeping them current. We surely keep an eye toward avoiding unnecessary x-rays. Every individual patient has a mutually agreed upon formula in reference to the frequency of needed x-rays.
Third molars are the most commonly removed teeth in our office. Both doctors remove teeth but Dr. Kimball is more often our choice. He is experienced and proficient with removing most of the teeth our patients need removed. Always focused on our patients’ better interest, we continue to refer appropriate removals to the care of an oral surgeon. Our patients surely participate in this decision.
Post orthodontically retention is mandatory. Fixed lingual (tongue side) retainers with a metal wire from cuspid to cuspid is the gold standard. We bond this wire onto the lower six anterior teeth requiring floss threading in five spaces. Removable tray retainers are our backups for those opposed to the hygiene challenges of the fixed lingual wire. Trays require compliance, the wire does not. We also utilize tray retainers to preserve the spatial relationship of teeth for our implant patients needing to delay treatment.
Short of periodontal surgery, scaling and root planing provides the therapeutic, nonsurgical alternative. In the presence of the inflammation involved with 5mm and 6mm pockets, local anesthesia allows our hygienists to clean more deeply and thoroughly. The antimicrobial rinse chlorhexadine is used before, during, and following scaling and root planing. Scaling and root planing, followed by adequately frequent periodontal maintenance appointments and good home care form the pragmatic triad to best avoid surgery. This overall nonsurgical program is termed Soft Tissue Management. To keep from sliding back into problem pocketing, scaling and root planing may need to be repeated every few years.
We place pit and fissure sealants in the chewing surface grooves of adult molars. This is done as the six and twelve year molars erupt, usually by age fifteen. Sealants are more important when the grooves are steep and prone to retaining food particles and bacterial plaque. Sealants are a mechanical barrier to limit, even prevent decay. Sealants are also appropriate on occasion for our more mature patients. To ensure we do not seal over decay, we beforehand confirm its absence by utilizing the laser fluorescence technology of Diagnodent. (See our blog concerning Diagnodent)
The free resin system material mentioned in the topic of removable partial dentures is quite versatile. Sectional partial dentures are also removable and can be utilized unilaterally. They may replace one to a few teeth on either side of the involved arch. Unilateral means only on one side, no connection under the tongue or across the palate, just a segment. (See Free Resin System Partial Dentures)
Leaving full scale orthodontics to our wonderful orthodontic collegues, we offer simple orthodontic correction for better anterior function, hygiene and cosmetics. We utilize strong, clear trays made by our orthodontic lab to uncrowd, rotate or close gaps for anterior teeth.
Snoring and sleep apnea are most frequently treated by physicians with a continuous positive air pressure machine or, “CPAP.” These machines involve masks or nasal cannula strapped to the skull, using significant air pressure to maintain the airway. There is the need of an electrical generator/electricity and maintaining “parts.” We, in collaboration with the treating physician, offer an alternative through providing an oral appliance. This dental appliance is carefully titrated to position the mandible in a slightly open, slightly forward position, pulling the otherwise relaxed tongue muscles with it. This movement of tongue muscles opens the airway and most often resolves both snoring and sleep apnea. Dr. Parker is a member of the American Association of Dental Sleep Medicine and continues his studies of what goes on when we sleep. Statistics confirm only 50% of our population can comply with a CPAP by the end of the first year of use. The far less invasive sleep disturbance appliance is well suited for patients of this profile.
The same homemade formula and passion of bruxism splints go into these splints. The TMJ splint is more directed toward relieving muscular pain (tension headaches) and reducing pressure at the temporomandibular joint (TMJ) than just protecting against tooth wear. Through careful equilibration or bite adjustment of the splint, we are able to posture the mandible correctly in the socket of the temporalis bone, at the TMJ. This is a muscularly relaxed position separate from where the bite directs the mandible. Allowing the mandible go to this muscularly relaxed position helps break the cycle of tension. TMJ splints are extremely valuable to a good number of our patients and require more precision than bruxism splints. In more acute cases, muscle relaxation splint therapy is combined with short term muscle relaxing or minor tranquilizing prescriptions. (See Bruxism Splint)
 Our entire staff is excited with the Kör Deep Bleaching system that Dr. Parker has brought into our office. After a couple of decades of professional whitening that has been less than predictable, we have found the source that puts “wow” into our whitening.
Our entire staff is excited with the Kör Deep Bleaching system that Dr. Parker has brought into our office. After a couple of decades of professional whitening that has been less than predictable, we have found the source that puts “wow” into our whitening.
The science behind this better method starts with trays that fit the teeth much more precisely than the trays we’ve been utilizing. These upgraded trays are made off premises by a dedicated laboratory. Trays now have a better seal at the gumline due to a far more precise impression process.
Besides trays with a better seal at the edge, the Kör Deep Bleaching system is also more successful because of superior whitening gels. Whitening agents from this system are much more closely controlled than prior systems. From the moment the whitening agents are manufactured, until the moment you load them into your trays, they are refrigerated and thus more predictably active. Refrigeration also allows the exclusion of the preservatives in more common gels that lead to sensitivity. Should sensitivity occur, we can conquer it or reduce it to acceptable levels.
Finally, we can take on those darker cases of intrinsic stain such as tetracycline; fluorosis, white spots, dark spots and “geriatric yellow”.
We are proud to be one of the few offices in Austin providing Kör Deep Bleaching.
For interim cosmetic remedy, usually after extraction of an anterior tooth, these nice looking removable appliances are worn while healing and tissue remodeling occurs. Typically transitional partial dentures also known as “flippers” are worn for a few months. They help somewhat with function but primarily are for esthetic purposes. With proper prior planning, they can be delivered at the same appointment the tooth is removed.
